
Gingivitis is inflammation of the gums (gingivae).
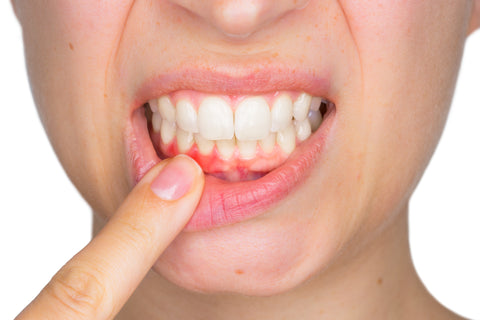
Gingivitis is an extremely common disease in which the gums become red and swollen and bleed easily. Gingivitis causes little pain in its early stages and thus may not be noticed. However, gingivitis that is left untreated may progress to periodontitis, a more severe gum disease that can result in tooth loss.
Gingivitis is divided into two categories:
-
Gingivitis due to plaque
- Gingivitis not due to plaque
Gingivitis Due to Plaque
Almost all gingivitis is due to dental plaque (a filmlike substance made up primarily of bacteria). By far, the most common cause is
Without adequate brushing, plaque remains along the gumline and builds up between the gums and the teeth (gingivitis does not occur in places where teeth are missing). Plaque also accumulates in faulty fillings and around the teeth next to poorly cleaned partial dentures, bridges, and orthodontic appliances. When plaque stays on the teeth for more than 72 hours, it can harden into tartar (calculus), which cannot be completely removed by brushing and flossing.
Plaque irritates the gums and creates pockets between the teeth and gums. Bacteria living in these pockets may cause gingivitis as well as cavities in the roots of the teeth. The gums appear red rather than a healthy pink. They swell and become movable instead of being firm and tight against the teeth. The gums may bleed easily, especially while brushing or eating. People usually do not have pain.
Gingivitis due to plaque can be prevented with good oral hygiene—the daily use of a toothbrush and dental floss. Some mouthwashes also help control plaque. After tartar forms, it can be removed only by a dentist or dental hygienist. People typically need professional cleanings (called scaling and prophylaxis ["prophy"]) every 6 to 12 months. However, people with poor oral hygiene, medical conditions that can lead to gingivitis, or a tendency to develop plaque more quickly than usual may need professional cleanings more often. Because of their excellent blood supply, gums quickly become healthy again after tartar and plaque are removed, as long as people brush and floss carefully.
In addition to poor oral hygiene, gingivitis due to plaque may also be started or worsened by
-
Drugs
-
Vitamin deficiencies
-
Hormone changes
-
Leukemia and leukopenia (low white blood cell count)
-
Diabetes
-
AIDS

Gingivitis Not Due to Plaque
Gingivitis that is not caused by plaque occurs in a small percentage of people. Causes include infections, allergies, disorders, and injuries.
Gingivitis due to infections
Viral infections can cause gingivitis. Acute herpetic gingivostomatitis is a painful viral infection of the gums and other parts of the mouth caused by the herpes virus. The infection turns the gums bright red and causes many small white or yellow sores to form inside the mouth.
Acute herpetic gingivostomatitis usually gets better in 2 weeks without treatment. Intensive cleaning does not help, so a person should brush gently while the infection is still painful. Dentists may recommend an anesthetic mouth rinse to relieve discomfort while eating and drinking.
Fungal infections can cause gingivitis as well. Fungi commonly grow in the mouth in very small amounts. Use of antibiotics or a change in overall health can increase the number of fungi in the mouth. Thrush (candidiasis) is a fungal infection in which the overgrowth of fungi, particularly Candida albicans, forms a white or red patch that irritates the gums. Patches can also coat the tongue and corners of the mouth and leave a bleeding surface if wiped away.
Thrush can be treated with an antifungal drug, such as nystatin, in the form of a mouth rinse or a lozenge designed to dissolve slowly in the mouth. Dentures should be soaked overnight in nystatin solution as well. Good oral hygiene (proper brushing and flossing) and treatment of underlying dental problems, such as ill-fitting dentures, can also help.

Gingivitis due to an impacted tooth (pericoronitis)
Gingivitis can develop in the gums surrounding the crown of an impacted tooth (a tooth that has not fully emerged). In this condition, called pericoronitis, the gum swells over the tooth that has not fully emerged. The flap of gum over the partially emerged tooth can trap fluids, bits of food, and bacteria.
Pericoronitis most commonly occurs around wisdom teeth (3rd molars), particularly the lower wisdom teeth. If the upper wisdom tooth emerges before the lower one, it may bite on this flap, increasing the irritation. Infections can develop and spread to the throat or cheek. The flap disappears once the tooth has fully emerged.
When people have pericoronitis, dentists may flush salt water under the flap of gum to rinse out the debris and bacteria. Sometimes, people are instructed to rinse at home with salt water, hydrogen peroxide, or the antiseptic chlorhexidine. If x-rays show that a lower tooth is not likely to emerge completely, dentists may remove the upper tooth and prescribe antibiotics for a few days before removing the lower one. Sometimes dentists remove the lower tooth immediately.
Oil Pulling With Coconut Ozonated Oil Can Transform Your Dental Health
The practice of “oil pulling” has been used for thousands of years to pull toxins from gum tissue in the mouth. It’s a mainstay tool of Ayurvedic Medicine and many people swear by its benefits. But now we’ve taken oil pulling into the 21st century with the addition of an ozone infusion right into the oil.
Ozone, the same elemental molecule you can smell in the air after a lightning storm, is now being used to radically transform modern dentistry. What dentists have discovered is that ozone kills bacteria throughout the mouth, including in tiny, microscopic crevices. Today, more and more dentists have become aware that old root canals may harbor dangerous bacteria and release toxins into the mouth which get swallowed into the body.

Oil pulling works far better than mouthwashes because oils are far better at penetrating all the tiny crevices and small areas around your gum tissue and teeth. If you’ve ever had a jar of coconut oil leak or spill, you know how coconut oil gets into everything, finding even the smallest opening to work its way through.
That’s why we chose coconut oil as the base oil for our oil pulling solution: it’s simply the best-performing oil available in the world for oil pulling.
Next, we infused it with ozone, creating an oil with outstanding penetration and ozone-carrying capacity. The ozone rides with the oils, reaching every microscopic gum line, tooth crack or fissure anywhere in your mouth, delivering bacteria-killing ozone to all those areas as you swish the oil around your mouth each morning.

Oil Pulling Instructions
- Put 1-2 teaspoons of ozonated oil into the mouth. The oil traditionally used in oil pulling is ozonated coconut oil. It is also possible to do oil pulling with ozonated olive oil. Whichever oil you choose, place 1-2 teaspoons in the mouth.
- Swish for 20 minutes. Apparently the timing is key, according to Dr. Bruce Fife, author of Oil Pulling Therapy, as this is long enough to break through plaque and bacteria but not long enough that the body starts re-absorbing the toxins and bacteria. The ozonated oil will get thicker and milky as it mixed with saliva during this time and it should be creamy-white when spit out. It will also double in volume during this time due to saliva.
- Spit oil into the trash can. The oil may thicken and clog pipes. Do not swallow the oil as it is hopefully full of bacteria, toxins and pus that are now not in the mouth!
- Rinse well with warm water. Warm water seems to clean the mouth better. We recommend you to rinse a few times with warm water to get any remaining oil out of my mouth. Some sources recommend swishing with warm salt water.
- Brush well!







Muchas gracias. ?Como puedo iniciar sesion?